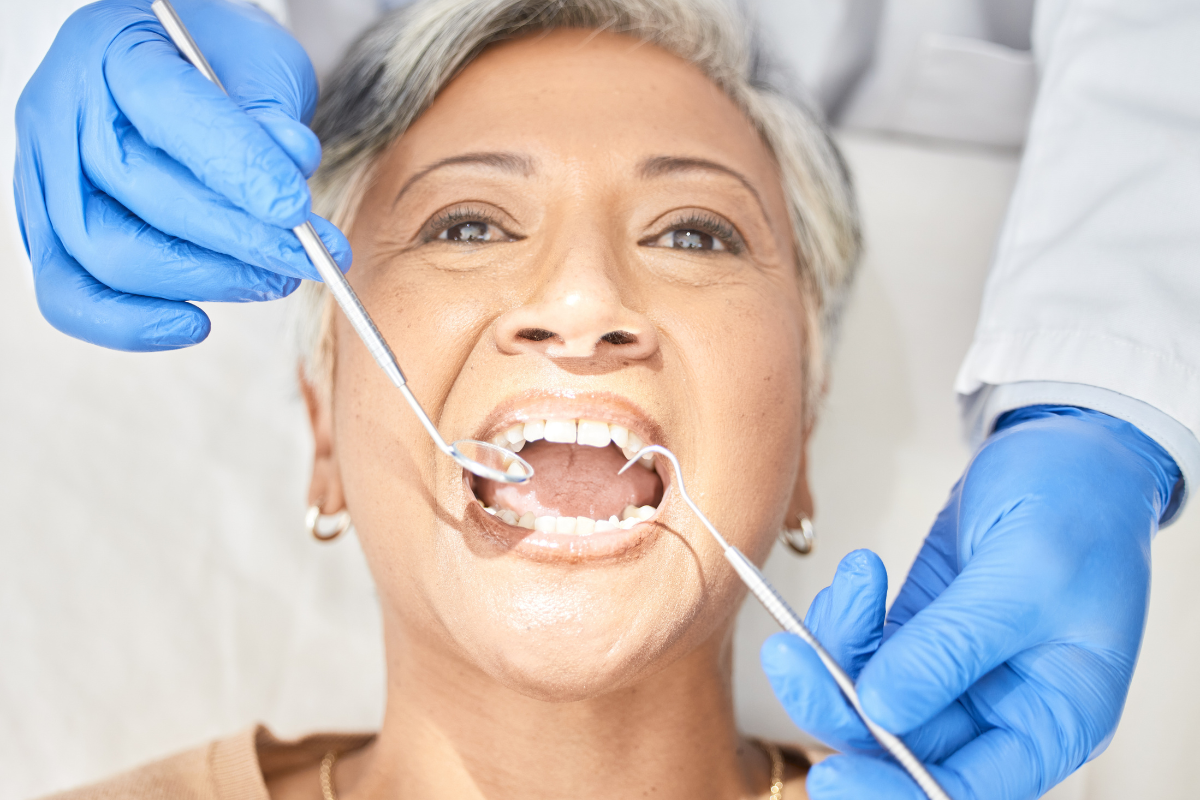
If you’ve ever had a sudden toothache in the middle of the night or woken up with a swollen jaw, you know how alarming dental emergencies can be. One of the first questions people ask is, “Will I need antibiotics?” It’s a fair question. But the answer isn’t always a simple yes. Understanding when antibiotics are truly needed, and when they aren’t, can help you make smarter decisions about your dental health.
What Counts as a Dental Emergency?
A dental emergency is any situation that causes severe pain, swelling, or risk of infection that needs prompt attention. Common emergencies include:
- A knocked-out or cracked tooth
- A painful abscess or swollen gum
- A severe toothache that doesn’t ease up
- Facial swelling that spreads toward the neck or eye
When patients visit an emergency dentist in Glendale for these issues, the dentist first assesses whether an infection is present and whether it’s spreading. That assessment drives the decision about antibiotics.
Why Antibiotics Are Not Always the First Answer
Many people assume antibiotics are the go-to fix for dental pain. In reality, antibiotics treat bacterial infections. They do not treat pain caused by nerve damage, a cracked tooth, or a cavity alone.
Giving antibiotics when they aren’t needed creates antibiotic resistance, a growing health concern. This means the bacteria become harder to treat over time. Responsible dentists only prescribe antibiotics when there’s a clear sign of bacterial infection, especially one that is spreading or risks becoming serious.
When Antibiotics Are Prescribed in Dental Emergencies
There are specific situations where antibiotics are necessary and appropriate.
Dental Abscess With Spreading Infection
A dental abscess is a pocket of pus caused by a bacterial infection. If the swelling spreads to the face, neck, or floor of the mouth, antibiotics are prescribed right away. This type of infection can become life-threatening if left untreated.
Infection in Patients With Weakened Immune Systems
Patients with diabetes, heart conditions, cancer, or those on immunosuppressant medication may need antibiotics even for minor dental infections. Their bodies are less able to fight bacteria on their own.
Post-Surgical Infections
After a tooth extraction or oral surgery, some patients develop infections. If signs of infection appear, such as increasing pain, swelling, or fever after the procedure, antibiotics help prevent the infection from worsening.
Cellulitis or Ludwig’s Angina
These are serious bacterial infections that spread through soft tissue. They require immediate treatment, often in a hospital setting, and always involve antibiotics as part of care.
Common Antibiotics Used in Emergency Dental Care
Dentists in Glendale typically prescribe one of the following antibiotics for dental infections:
Amoxicillin is the most commonly used antibiotic for dental infections. It works well against the bacteria found in the mouth and is well tolerated by most patients.
Amoxicillin-Clavulanate (Augmentin) is used when the infection is more resistant or hasn’t responded to amoxicillin alone.
Clindamycin is prescribed for patients who are allergic to penicillin. It’s effective for many oral bacterial infections.
Metronidazole is sometimes added to treat infections involving anaerobic bacteria, which thrive in low-oxygen environments like deep gum pockets.
Your dentist will choose based on your health history, allergies, and the type of infection present.
What Happens If You Skip Antibiotics When You Need Them?
Dental infections don’t go away on their own. If left untreated, a bacterial infection in the mouth can spread to the jaw, neck, or even the brain. This can lead to hospitalization, surgery, or worse.
If your emergency dentist in Glendale recommends antibiotics, it’s because the infection needs to be controlled before or after dental treatment. Completing the full course of antibiotics matters too. Stopping early, even if you feel better, allows surviving bacteria to regrow and become resistant.
Antibiotics Are a Support, Not a Solution
This is a key point many patients miss. Antibiotics manage the infection, but they don’t fix the source. A tooth with an abscess still needs a root canal or extraction. An infected gum still needs to be cleaned and treated.
Think of antibiotics as clearing the path so the dentist can safely treat the real problem. Without addressing the source, the infection will return.
Local Considerations for Residents Seeking Urgent Dental Care
In Glendale, Arizona, dental emergencies can come up without warning, especially during extreme heat months when people may be more prone to dehydration, which affects oral health. Dry mouth raises the risk of bacterial growth and tooth decay, sometimes leading to sudden infections.
Having access to an emergency dentist in Glendale means you don’t have to wait days for care. Prompt treatment reduces the chance that a minor infection becomes a major one requiring stronger medication or hospitalization.
Many residents in the Glendale area also face challenges related to access and awareness around when to seek care. The rule of thumb is simple: if you have swelling, fever, or pain that isn’t going away, don’t wait.
Tips for Managing Dental Pain Before Your Appointment
While waiting to see your dentist, here are a few safe steps:
- Rinse with warm salt water to reduce bacteria in the mouth
- Take over-the-counter pain relief like ibuprofen to manage discomfort and inflammation
- Avoid hot or very cold foods that may trigger more pain
- Do not place aspirin directly on the gum, as it can cause burns
These steps won’t treat the infection, but they can make you more comfortable until you receive proper care.
Conclusion
Antibiotics play an important role in emergency dental care, but only when they are truly needed. They work best when prescribed for the right reason, at the right time, and for the full course of treatment. Misusing them does more harm than good.
If you’re dealing with a dental emergency and are unsure whether you need antibiotics, a dentist in Glendale can help you get a proper diagnosis and the right treatment plan. Early action is always the best choice. Waiting too long can turn a manageable problem into a serious health concern.
At Family Dental Station in Glendale, Arizona, the team is ready to help you through dental emergencies with clear, honest care. If you’re in pain or have concerns about a possible infection, schedule a consultation with Family Dental Station to get the care you need without delay. You can also contact our glendale dentist office directly to ask questions or book an urgent appointment.
Your health is worth acting on quickly.
Frequently Asked Questions
1. Will my dentist always prescribe antibiotics for a tooth infection?
No. Antibiotics are only prescribed when there’s a true bacterial infection, especially one that’s spreading. Many dental infections are treated through procedures like drainage or root canal without antibiotics.
2. How long does it take for antibiotics to work on a dental infection?
Most patients begin to feel improvement within 24 to 48 hours. The full course, usually 5 to 7 days, must be completed even if symptoms improve early.
3. Can I get antibiotics without seeing a dentist?
No. Antibiotics for dental infections require a prescription from a licensed dentist or doctor. Self-medicating is not safe and can lead to resistance.
4. What should I do if I’m allergic to penicillin?
Tell your dentist before any prescription is written. Alternatives like clindamycin are available and effective for most dental infections.
5. Is it safe to take antibiotics if I’m pregnant?
Some antibiotics are safe during pregnancy and some are not. Your dentist will consult with your doctor or OB-GYN before prescribing anything. Always disclose your pregnancy at the start of the appointment.
6. Why do I still have pain after starting antibiotics?
Antibiotics treat the infection, not the pain. The source of the problem, such as an abscess, still needs dental treatment. Pain should be managed with approved over-the-counter medication until your procedure.
7. Can a dental infection go away on its own without treatment?
No. Bacterial dental infections do not resolve without treatment. Waiting makes them worse and raises the risk of the infection spreading beyond the mouth.
8. What signs mean I need emergency dental care right away?
Go in immediately if you have facial swelling, difficulty swallowing or breathing, a fever above 101°F, or severe throbbing pain that is getting worse. These may signal a spreading infection that requires urgent care.