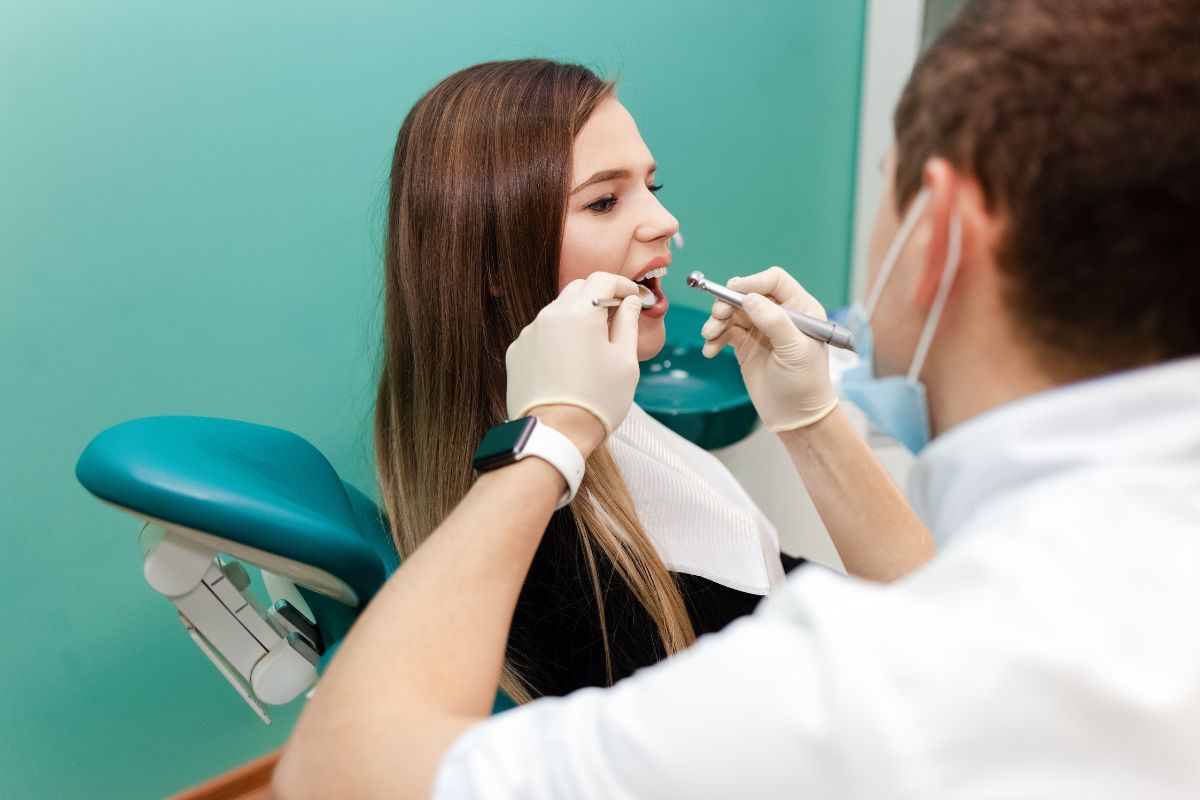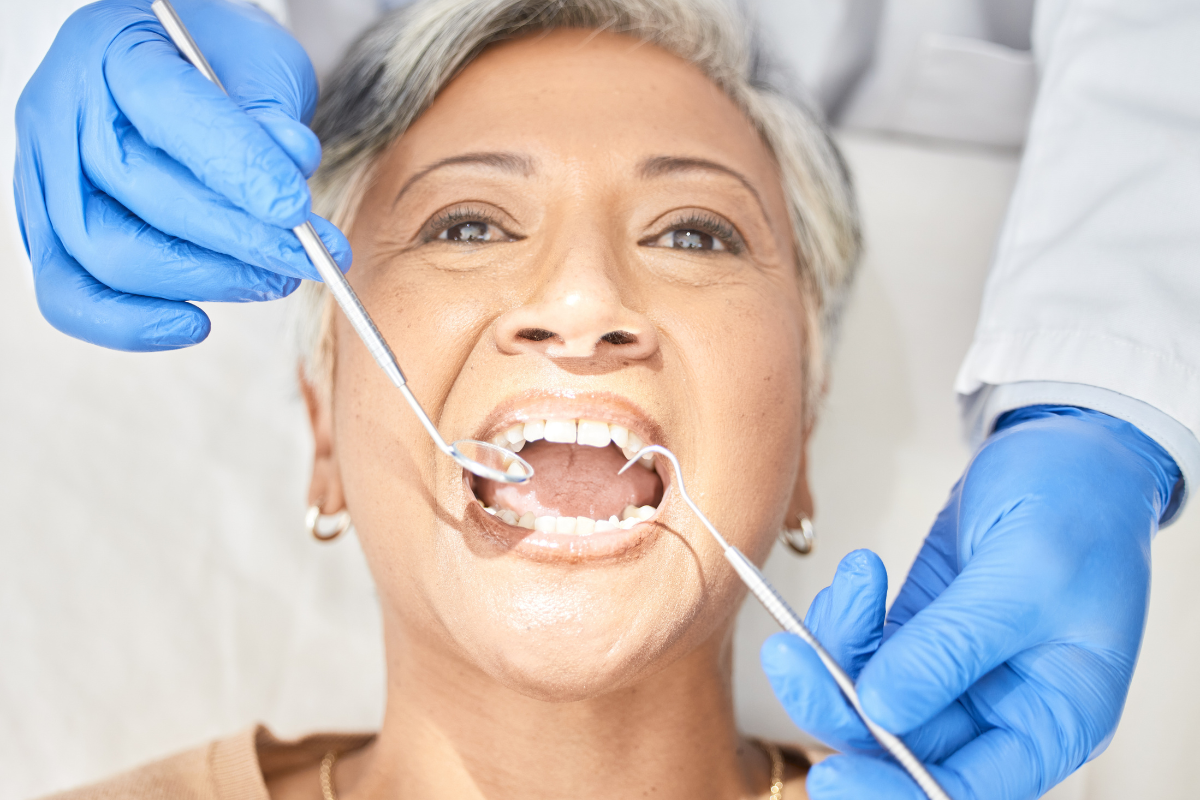
When a tooth becomes severely damaged or infected, extraction may be the only real option left. It is a situation that causes a lot of anxiety for most people. But knowing what the process actually looks like can make a big difference in how you handle it.
Whether you are dealing with sudden dental pain right now or just want to be prepared, this guide walks you through everything clearly.
When Is a Tooth Extraction Actually Necessary?
Not every toothache leads to extraction. Dentists always try to save a natural tooth first. But there are situations where pulling the tooth is the safest path forward.
Common reasons a dentist may recommend extraction include:
- A tooth that is too broken to repair with a crown or filling
- Severe infection that has not responded to antibiotics or a root canal
- Advanced gum disease that has loosened the tooth at its root
- An impacted wisdom tooth causing pain or crowding
- A tooth causing problems before orthodontic treatment
If you are searching for a dentist in Glendale and dealing with any of these issues, getting seen quickly matters. Delaying treatment can allow an infection to spread beyond the tooth and into surrounding tissue.
What Happens During an Emergency Extraction?
The procedure itself is more straightforward than most people expect. Here is a simple breakdown of what typically takes place.
Step 1: Examination and X-Ray
Before anything else, the dentist takes an X-ray to understand the tooth’s root structure and the extent of damage. This step guides the entire procedure.
Step 2: Local Anesthesia
The area around the tooth is numbed with a local anesthetic. You will feel pressure during the procedure but not sharp pain. Most patients are surprised by how comfortable this part is.
Step 3: The Extraction
For a simple extraction, the dentist loosens the tooth using a tool called an elevator, then removes it with forceps. The process usually takes just a few minutes.
For a surgical extraction (common with impacted teeth or broken roots), a small incision in the gum may be needed. This takes a bit longer but is still done under local anesthesia.
Step 4: Gauze and Clotting
Once the tooth is out, the dentist places gauze over the socket and asks you to bite down to help a blood clot form. This clot is critical for healing.
Does It Hurt? Let’s Be Honest
During the procedure, the anesthesia does its job well. You may feel the tooth being moved, but pain is not something most patients report while sitting in the chair.
After the anesthesia wears off (usually two to four hours later), some soreness and swelling are normal. For most people, over-the-counter pain relievers like ibuprofen manage this effectively.
The first 24 to 48 hours are the most uncomfortable. Pain should steadily decrease after that. If it is getting worse instead of better by day three or four, that is a sign to call your dental office right away, as it may indicate a dry socket or infection.
Recovery: What to Do (and Not Do)
Recovery from a tooth extraction is manageable when you follow a few simple guidelines.
Do:
- Keep biting on gauze for 30 to 45 minutes after the procedure
- Apply an ice pack to your cheek for 10-minute intervals to reduce swelling
- Eat soft foods like yogurt, mashed potatoes, soup, and smoothies for the first few days
- Take prescribed or recommended pain medication as directed
- Rest for the remainder of the day
Do Not:
- Smoke or use tobacco products for at least 72 hours
- Drink through a straw (the suction can dislodge the clot)
- Rinse aggressively or spit forcefully for the first 24 hours
- Eat hard, crunchy, or very hot foods near the extraction site
- Poke the socket with your tongue or fingers
Most people return to normal activities within two to three days. Full tissue healing usually takes one to two weeks.
What Is Dry Socket and How Do You Avoid It?
Dry socket happens when the blood clot that forms in the socket is dislodged or dissolves too early. This exposes the bone underneath, which is painful.
Signs of dry socket include a throbbing ache that starts two to three days after extraction, bad breath, and a visible empty-looking socket.
It is more common in smokers, people who did not follow aftercare instructions, or those with lower immune function. If you think you have dry socket, do not wait. A dentist near me or dentist in glendale search can help you find same-day care if needed. Your dentist will place a medicated dressing to ease the pain and protect the socket while it heals.
When to Consider Tooth Replacement
Losing a tooth does not have to be permanent. Once the socket heals (usually after a few months), replacement options are available.
The most common options include:
- Dental implants: A titanium post placed in the jawbone, topped with a crown. The closest thing to a natural tooth.
- Dental bridges: A false tooth held in place by crowns on the adjacent teeth.
- Partial dentures: A removable option for replacing one or more missing teeth.
Talking to a dentist in Glendale early about replacement options helps you plan ahead and avoid bone loss in the jaw over time.
Frequently Asked Questions
1. How long does a tooth extraction take?
A simple extraction usually takes 20 to 40 minutes, including preparation. Surgical extractions may take longer depending on the complexity.
2. Can I eat before an emergency extraction?
For a simple extraction with local anesthesia, eating beforehand is generally fine. Your dental office will give you specific instructions based on your situation.
3. How do I manage pain after extraction at home?
Ibuprofen or acetaminophen works well for most patients. Take as directed. Ice packs during the first 24 hours also help reduce swelling.
4. When should I call my dentist after an extraction?
Call if you have bleeding that does not stop after an hour, increasing pain after day two, fever, swelling that gets worse, or signs of infection like pus or a bad taste.
5. Is it safe to get a tooth pulled when I have an infection?
Yes, in many cases. Dentists often use antibiotics to reduce infection before or after extraction. Leaving an infected tooth in place is often more dangerous.
6. What if I am nervous about the procedure?
It is very common to feel anxious. Tell your dental team before the appointment. Many offices offer options to help you feel more at ease during treatment.
7. How soon can I return to work after extraction?
Most people feel comfortable going back to a desk job the next day. If your work is physically demanding, you may want to take an extra day to rest.
8. Will I need stitches after extraction?
Not always. Stitches are more common after surgical extractions. If placed, they are usually dissolvable and do not require a separate removal visit.
A Note for Local Residents
Dental emergencies do not follow a schedule. For those living in and around the Glendale, Arizona area, having a trusted local dental office you can call matters. Hot summers, busy schedules, and access to fast food are all part of life here. These factors can contribute to dental problems that build up quietly until they become urgent.
At Family Dental Station, we understand the pace of life in this community. We are here to provide fast, compassionate care when you need it most, without making you feel rushed or judged.
Conclusion
A tooth extraction is not something anyone looks forward to. But when it is necessary, understanding the process takes away a lot of the fear. The procedure is quick, the pain is manageable, and recovery is something most people handle well with proper care.
If you are in pain right now or have been putting off a dental visit, do not wait for things to get worse. Search for a dentist near me to find immediate help, or reach out directly to us. Schedule a consultation with Family Dental Station to get a clear picture of your options. Contact our Family Dental Station office today, and let us help you move past the pain and toward better dental health.